Inclusion Health
Inclusion health is an umbrella term used to describe people who are socially excluded, who typically experience multiple interacting risk factors for poor health, such as stigma, discrimination, poverty, violence, and complex trauma.
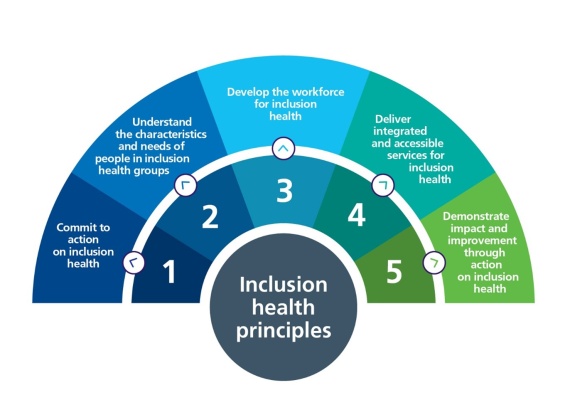
Inclusion health focuses on the healthcare needs of people who face serious social disadvantages and are often excluded from regular healthcare services. These individuals usually encounter many barriers when trying to access healthcare, leading to negative experiences that discourage them from seeking medical help in the future. As a result, they are less likely to get the care they need, despite having high health needs. This contributes to poorer health outcomes and a shorter life expectancy compared to the general population.
The poor health of inclusion health groups is mainly due to their severe social disadvantages and the build-up of various social risks. For example, someone who is alcohol-dependent might also be homeless, making them very vulnerable and limiting their chances for better health. This combination of factors leads to very poor health and a shorter life expectancy. Additionally, bad experiences during childhood can lead to social exclusion and increased health needs throughout a person’s life.
To effectively reduce healthcare inequalities, it is crucial to have a clear and focused approach to addressing the needs of inclusion health groups.
People in inclusion health groups include:
- People who experience homelessness
- People with drug and alcohol dependence
- Vulnerable migrants and refugees
- Gypsy, Roma, and Traveller communities
- People in contact with the justice system
- Victims of modern slavery
- Sex workers
- Other marginalised groups
People who are socially excluded are likely to have the following experiences in common:
- Discrimination and stigma
- Violence and the experience of trauma
- Poverty
- Invisibility in health datasets
Which result in:
- Insecure and inadequate housing
- Very poor access to healthcare services due to service design
- Poor experience of public services
- Poorer health than people in other socially disadvantaged groups.
Further resources:
NHS England Inclusion Health Guidance and Framework
All Our Health Inclusion Health eLearning
The effect of multiple adverse childhood experiences on health: a systematic review
Gypsy, Roma and Traveller communities
Romany Gypsy, Roma and Irish Traveller communities are known to face some of the starkest inequalities in healthcare access and outcomes amongst the UK population, including when compared with other minority ethnic groups. The reasons for these poor health outcomes are complex, but include the impact of discrimination and stigmatisation, the complicated nature of health systems and the effects of wider social determinants of health.
Key inequalities:
- Romany and Traveller people face life expectancies between ten and 25 years shorter than the general population.
- Romany and Traveller people experience significantly higher prevalence of long-term illness, health problems or disabilities, which limit daily activities or work.
- The health of a Romany or Traveller person in their 60s is comparable to an average White British person in their 80s.
- An All Ireland study found that suicide prevalence is six times higher for Irish Traveller women than women in the general population, and seven times higher for Traveller men.
- 60% of Roma Support Group’s migrant Roma beneficiaries are reported to have poor physical health, with 43% of Roma beneficiaries of the above reported to suffer from poor mental health.
Key Issues:
There are a number of factors that contribute to poor health outcomes among Gypsy, Roma and Traveller communities. These relate to structural inequalities, social exclusion, and barriers to healthcare services. Key issues include:
- Chronic exclusion across the wider determinants of health.
- Invisibility in mainstream datasets, meaning needs aren’t identified within services.
- Lack of trust in services as a result of fear of and experiences of discrimination.
- Wrongful registration refusal in primary care.
- Digital exclusion and lack of accessible information.
- Inequalities in access to healthcare waiting lists for nomadic populations.
- Inequalities in mental health and access to mental healthcare.
- A failure within services to account for premature onset of typically age-related conditions.
[Source: Friends, Families & Travellers]
Awareness & Training Resources:
Tackling inequalities faced by Gypsy, Roma and Traveller communities - Report Summary: A House of Commons report with recommednations to the govenment to address health inequalities.
Friends and Families Travellers webinar: Introduction exploring key issues and place based approach within NHS South East.
Friends, Families & Travellers Teaching Resources: Downloadable and practical content to support educational settings.
Friends, Families & Travellers Training Packages: Digital courses that provides greater understanding of the diversity, barriers and available information to enable inclusive services.
Traveller Movement Education Microsite: online guidance for Travellers seeking guidance as well as organisations looking to improve their engagement offer.
Traveller Movement Safe Space for Women Microsite: Providing information and support for Gypsy Roma and Traveller women.
York Travellers Trust: Charity seeking to reduce inequalities and fight discrimination
East Riding of Yorkshire Council Gypsy and Traveller sites: Facilities and support available from East Riding of Yorkshire Council.
ONS Lived Experience Report: Qualitative research exploring the lived experiences of Gypsy and Traveller communities, relating to education and employment.
Travellers Times Relationship and Education: website creating content for the traveller community






